
Beating bunions
Are you in pain from bunions and considering surgery? We answer common questions, with advice from consultant trauma and orthopaedic surgeon Mr Adam Ajis from Goring Hall Hospital.
Although there are ways you can manage bunion symptoms, the only way to fix them is to have an operation. If your bunions are affecting your quality of life, it may be time to consider surgery.
Did you know that around 15% of women in the UK suffer from bunions?
What are bunions?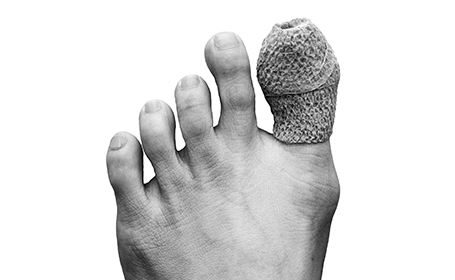
Bunions, also known as hallux valgus, are hard lumps that form on the outside of your feet, at the base of your big toes.
They happen when the big toe angles too much towards the second toe, leading to a bony lump at the joint. You may feel pain in this lump and along the side or bottom of your feet.
What causes bunions?
Bunions are thought to be genetic, with certain foot shapes being more prone to them. If members of your family have suffered from bunions, you may also develop them.
Genetic predisposition is the only real cause of bunions, even though many people believe that ill-fitting shoes are to blame. In reality, some people are simply prone to bunions. If this is the case, ill-fitting footwear might encourage the development of bunions. Tight or narrow shoes can squeeze and crowd the toes and exacerbate existing problems. However, many people would be able to wear poorly fitted shoes and never develop bunions.
If your bunions are getting worse or are getting in the way of your normal activities, you should visit your GP or a foot specialist.
What treatments are available for bunions?
Some people find bunions don't cause them much discomfort, but others find they are very painful and unsightly.
There are some at-home bunion treatments that can ease or manage the symptoms, including ice packs, bunion pads and making sure to wear comfortable, well-fitting footwear. However, these methods won't work for everyone.
If your bunions are getting worse or are getting in the way of your normal activities, you should visit your GP or a foot specialist.
A foot specialist might recommend orthotics, which are devices that modify the position of your toes and feet in general, with the aim of reducing pain and improving function. A silicone spacer between the big toe and second toe can be very effective at reducing rubbing.
Another option is splints that straighten the big toe using the rest of the foot as a splint. These do not prevent bunions occurring, but they can reduce the ache. Orthotics can also fit inside your shoe replacing the insert or lining to modify how your foot makes contact with the ground. These can be bought in a chemist or made specifically for you by an Orthotist or Podiatrist.
When is bunion surgery recommended?
Surgery is the only way to correct bunions, however it's usually only recommended when your bunions symptoms are very disruptive and other, conservative treatments haven't helped.
Our Consultant Trauma and Orthopaedic Surgeon Mr Adam Ajis specialises in conditions of the foot and ankle at Goring Hall Hospital. He shares his advice on bunion surgery and recovery:
It's worth discussing the various surgical options to help decide which is most appropriate for you.
What are the different types of bunion surgery?
"There are a lot of different types of bunion operations. These can include minimally invasive bunion surgery or open surgery. Each has its pros and cons and after a thorough consultation, taking your views and expectations on board, you and your consultant can come up with a plan together.
"It's worth discussing the various surgical options to help decide which is most appropriate for you. However, any type of bunion surgery will involve the surgeon making a carefully planned cut in the bone, moving it back to the correct position and holding it there with small screws until it all heals up."
How long will I be in the hospital?
"Bunion surgery is most often carried out under general (asleep) anaesthetic, though it is sometimes performed under local (awake) anaesthetic.
"If you have other conditions or if you are having multiple toes corrected, you may need to stay overnight. However, bunion surgery is routinely carried out as day case procedure. That means most people leave hospital the same day they have the operation.
"People are often able to put weight on the foot the same day of the procedure, though you'll need to be cautious. A special shoe can be worn to take pressure off the front of the foot.
"Bandages, dressings and sutures are typically removed after two weeks. By week six, an X-ray should be carried out to check on healing. By this time, you should be able to wear normal shoes again so long as they are roomy and comfortable."
Will I be in pain after surgery?
"There will likely be some pain, however your doctor or nurse will advise you on how to manage this with painkillers. There will also be some swelling. Swelling is the body's natural response to healing and repair. It's usually nothing to worry about, but it does need to be kept under control as it can become uncomfortable if left unchecked.
"Get up to speed with household tasks, stock the fridge, pre-cook meals… Anything to make your life easier while you're recovering."
What can I do to encourage healing?
"During the first six weeks, although full weight bearing is permitted, a good way to speed up healing is to rest and elevate the foot. The higher the better, but it should be at least higher than the level of your heart to reduce swelling. Keeping the toes moving while the foot is elevated helps prevent stiffness and can also keep swelling down.
"Relax and take it easy as much as possible. Deciding on a surgery date and planning ahead of it is essential to help you do this. As I advised above, get up to speed with household tasks, stock the fridge, pre-cook meals if necessary. Anything to make your life easier."
How long will recovery take?
"Most people should start to feel back to normal after six weeks, but everyone is different. Full recovery may take up to six months and you may still experience some swelling up to a year after surgery.
"Be sure to ask your doctor about physiotherapy. There may be exercises you can do to improve your strength and range of motion. These should encourage your recovery, though they won't always be necessary."
When can I go back to work?
"Returning to work is variable and dependant on your job, but it can be as soon as two weeks for sedentary occupations with certain types of procedures.
"Still, it can also be as long as 6-12 weeks before you're able to return. It's important to have realistic expectations.
"Your surgeon should be able to provide you with certificate for work advising how much time away is necessary."
When will I be able to drive again?
"If it's your right foot you won't be able to drive for six to eight weeks. If it's your left foot you can drive an automatic car after two weeks.
"After any surgery, you should contact your car insurance company before getting behind the wheel, just in case. Not all companies have the same policies."
What else should I know?
"There are often lots of questions that you don't think of at the time of consultation.
"Always make sure that you have a contact number or email address to get back in touch so your concerns can be addressed. This way, you can focus on being as relaxed and as comfortable as possible."

Tags
How do I book an appointment?
If you're concerned about symptoms you're experiencing or require further information on this subject, talk to a GP or see an expert consultant at your local Circle Hospital.